| Share |  |
 | |||
INFLAMMATION - the Fuel that Flames the Fire of Disease
 There is increasing recognition of the connection between inflammation and a host of common health problems people experience today. The root word for inflammation in Latin is “inflamatio”, which literally means, “to set on fire”. Many believe that chronic inflammation is the fuel that flames the fire of many of today’s degenerative diseases.
There is increasing recognition of the connection between inflammation and a host of common health problems people experience today. The root word for inflammation in Latin is “inflamatio”, which literally means, “to set on fire”. Many believe that chronic inflammation is the fuel that flames the fire of many of today’s degenerative diseases.
Inflammation is apparent in such conditions as arthritis, bronchitis, laryngitis, sinusitis, gastritis, colitis or appendicitis. After all, the suffix of these diseases named for the organ or site in which they occur, is “itis”, meaning “inflammation of…” However, a growing number of studies reveal that hidden systemic inflammation (that which affects the entire body or a particular body system) may be the common denominator linking many other modern diseases even when the connection may not be as obvious.
Evidence of Inflammation
Primary among these conditions is heart disease – the nation’s number one killer among women in this country. Cardiovascular disease is rapidly being redefined as an inflammatory disease of the blood vessels. Blood tests are available which measure levels of C-reactive protein (“CRP”), a protein molecule produced in the liver in response to inflammation. Elevated CRP levels can indicate a high degree of systemic inflammation in the body.
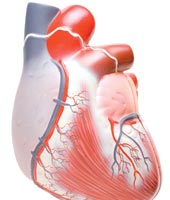 This clinical marker of inflammation is now deemed to be an even more accurate early indicator of the risk of heart disease than cholesterol or triglyceride levels. According to the American Heart Association, scientific studies have found that the higher the hs-CRP level (“hs” designates a “high sensitivity” type of CRP test), the higher the risks of having a heart attack. In a study done with a population of elderly people who were considered to be generally “healthy”, those who had the highest levels of CRP as well as Interleukin-6 (another marker of systemic inflammation) were 260 percent more likely to die within a four-year period than those with low levels of inflammatory markers.
This clinical marker of inflammation is now deemed to be an even more accurate early indicator of the risk of heart disease than cholesterol or triglyceride levels. According to the American Heart Association, scientific studies have found that the higher the hs-CRP level (“hs” designates a “high sensitivity” type of CRP test), the higher the risks of having a heart attack. In a study done with a population of elderly people who were considered to be generally “healthy”, those who had the highest levels of CRP as well as Interleukin-6 (another marker of systemic inflammation) were 260 percent more likely to die within a four-year period than those with low levels of inflammatory markers.
Studies also show that the longer a person exhibits elevated levels of CRP, the greater their chance of developing some form of chronic illness. The presence of inflammation, indicated by elevated CRP markers, is also found in those with other health conditions on the rise today, such as diabetes, cancer, Alzheimer’s, Parkinson’s, allergies, asthma, fibromyalgia, Irritable Bowel Syndrome, eczema, and autoimmune disease.
A Blessing in Disguise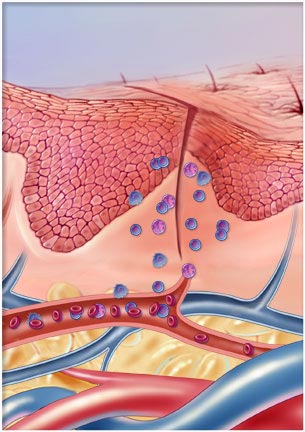 Not all inflammation is bad. Acute or short-term inflammation is actually the body’s natural self-healing response to trauma, infection or other irritants. It is generally caused by allergens, environmental toxins, insect bites, excess heat or radiation. This type of inflammation is the body’s initial reaction to cellular damage and serves to rally the immune system’s defense mechanisms to fight foreign invaders. It is designed as well to facilitate healing by repairing damaged tissue and removing any toxins or microbial debris from the body. Without the process of inflammation, the body would not be able to recover quickly from wounds and infections.
Not all inflammation is bad. Acute or short-term inflammation is actually the body’s natural self-healing response to trauma, infection or other irritants. It is generally caused by allergens, environmental toxins, insect bites, excess heat or radiation. This type of inflammation is the body’s initial reaction to cellular damage and serves to rally the immune system’s defense mechanisms to fight foreign invaders. It is designed as well to facilitate healing by repairing damaged tissue and removing any toxins or microbial debris from the body. Without the process of inflammation, the body would not be able to recover quickly from wounds and infections.
Acute inflammation is typically characterized by heat, redness, swelling or pain. Anyone who has cut his or her finger, sprained an ankle or had a sore throat knows what it is like to experience this type of inflammation. Although the body’s reaction may be unpleasant to experience, each stage of inflammation is vital for healing and tissue repair to occur. Here are examples of some of the stages that take place “behind the scenes” when the typical symptoms of an inflammatory response occur:
- Chemical signals are released by cells at the site of the injury, which attract white blood and other cells that fight infection
- Heat is produced by the increase of cellular activity as well as oxidation at the injury site
- Swelling occurs as blood vessels dilate to increase the flow of blood so that white blood cells can easily get to the damaged area to engulf and destroy any bacteria or debris that might cause or continue the inflammation
- Extra blood (which produces redness) carries antibodies to neutralize toxic substances and microorganisms. This blood also carries oxygen and nutrients to create new cells for repair of damaged tissue
- Pain, which serves to alert the injured person of the problem and protect the affected area from overuse, is due to both the swelling tissue putting pressure on nerves and a lack of oxygen to the injured tissues
In addition to these types of processes, many other biochemical reactions occur that involve the release of different chemical substances associated with the immune system and the regulation of inflammation.  Among these substances are different types of prostaglandins (a group of hormone-like substances that regulate various biological processes), some of which activate inflammation and others that work to shut it down once the function of the initial stages are complete. As long as the body still needs to work to destroy bacteria or counteract any offending trigger, these “pro-inflammatory” prostaglandins remain active.
Among these substances are different types of prostaglandins (a group of hormone-like substances that regulate various biological processes), some of which activate inflammation and others that work to shut it down once the function of the initial stages are complete. As long as the body still needs to work to destroy bacteria or counteract any offending trigger, these “pro-inflammatory” prostaglandins remain active.
When it comes to acute inflammation, the typical first-line treatments are anti-inflammatory drugs (NSAIDS) such as aspirin or ibuprofen. These medications effectively suppress inflammation by blocking key enzymes (COX 1 and COX-2) responsible for prostaglandins that tend to promote inflammation and pain in the body. This can provide a good benefit short term, but over the long term, these drugs can be harmful to the body. Besides having adverse side effects (including intestinal bleeding, kidney and liver damage), anti-inflammatory drugs and steroids have the distinct disadvantage of blocking both pro-inflammatory and anti-inflammatory prostaglandins, thus interfering with the body’s own immune response and ability to heal and repair itself.
When Is Inflammation Considered Chronic?
In a normal scenario, anti-inflammatory agents accomplish the job of destroying infectious agents, clearing away cellular debris and regenerating new tissue. If, however, the response of the anti-inflammatory compounds is not completely turned off, this constant low-grade flow of inflammatory components in the blood will result in prolonged tissue breakdown. In other words, tissues are continuously injured by infection, stress, or irritation in this situation, which results in chronic inflammation.  What begins as a normal healthy immune response turns into an out-of-control reaction that destroys cells and tissues of the body, paving the way for degenerative disease and rapid aging. In the case of autoimmune disease, the immune system response is thrown off to the point where, instead of attacking the source of the inflammation, it attacks and destroys perfectly healthy tissue.
What begins as a normal healthy immune response turns into an out-of-control reaction that destroys cells and tissues of the body, paving the way for degenerative disease and rapid aging. In the case of autoimmune disease, the immune system response is thrown off to the point where, instead of attacking the source of the inflammation, it attacks and destroys perfectly healthy tissue.
When the body has to constantly maintain a defensive posture, this hyperactive immune state and smoldering inflammation wears on the body’s energy and resources. The body’s ability to function optimally is impeded as organs and systems of the body gradually begin to break down. However, the damage produced by any inflammation is not generally noticed until it has reached a level significant enough to produce symptoms. This is why chronic inflammation is sometimes referred to as the “silent killer”.
Causes of Chronic Inflammation
It is important to identify triggers that can cause this type of inflammation. Some of the most common underlying causes of chronic inflammation are:
- Poor diet (sugar, refined flour, trans and hydrogenated fats)
- Nutrient Deficiencies (particularly B vitamins, Vitamin C, Vitamin D, zinc and omega-3 fats)
- Environmental allergens (pollens, molds, dust, etc.)
- Environmental toxins (such as mercury and pesticides)
- Food allergens – both immediate and delayed allergies – most common are wheat/gluten, dairy, eggs, yeast, corn, peanuts, citrus, soy, shellfish and tree nuts.
- Repeated infections or chronic low grade infection
- Lack of exercise/sedentary lifestyle
- Abdominal Fat
- Prolonged emotional stress or physical trauma
- Ongoing sleep deficiencies (averaging less than seven hours)
- Age related tissue breakdown
The Role of Diet
Since foods provide the nutritional building blocks for the body and its immune system, little doubt exists that the deteriorated state of the typical Western diet today is the primary underlying cause of degenerative disorders related to inflammation. Acute inflammation only turns into chronic inflammation when there are imbalances and low levels of nutrients in the diet. Most diets today contain twenty to thirty times more pro-inflammatory nutrients than a century ago. It takes the right mix of nutrients for the body to form the proper counterbalance between pro-inflammatory substances required to fight infection and irritants and anti-inflammatory substances needed to moderate and turn inflammation off at the appropriate time so that tissue healing and repair can begin.
The Right Balance of the Right Fats
Chronic inflammation often develops when there is significant imbalance in the type of fats consumed. Maintaining the proper ratio between omega-3 and omega-6 fats is key for enabling the body to produce the correct balance of pro-inflammatory and anti-inflammatory prostaglandins. The main dietary firefighter that works to restore balance and prevent or reverse chronic inflammation is omega-3 fatty acid.  This is because omega-3 ultimately converts to a group of prostaglandins that are either anti-inflammatory or less inflammatory than what omega-6 produces, whereas excess amounts of omega-6 shift the body towards chronic inflammation.
This is because omega-3 ultimately converts to a group of prostaglandins that are either anti-inflammatory or less inflammatory than what omega-6 produces, whereas excess amounts of omega-6 shift the body towards chronic inflammation.
A major reason for the shortage of anti-inflammatory omega-3 fats in the diets of most Americans is the widespread use of refined omega-6 vegetable oils along with hydrogenated and trans fats. There has been a drastic increase in the consumption of these processed oils and fats over the last one hundred years. They are used in nearly all commercially produced baked goods, in salad dressings and in just about every form of cooking that takes place in most restaurants and homes.
Even though the highly refined versions of these oils and hydrogenated fats are less prone to become rancid (thereby increasing shelf life) and can be heated at higher temperatures than omega-3 or omega-9 oils, their overuse greatly increases the production of pro-inflammatory prostaglandins. Not only that, but trans fats displace omega-3 essential fatty acids, interfering with the conversion pathway that leads to the production of anti-inflammatory prostaglandins.  For a more complete understanding on how the right balance of the omega fatty acids affects health and which oils and fats you should or shouldn’t use, I would encourage you to review my articles on “Understanding Fats – the Good, the Bad and the BEST” and “Healthful Cooking Oils” (April, May, 2009)
For a more complete understanding on how the right balance of the omega fatty acids affects health and which oils and fats you should or shouldn’t use, I would encourage you to review my articles on “Understanding Fats – the Good, the Bad and the BEST” and “Healthful Cooking Oils” (April, May, 2009)
An additional factor that explains the increase of omega-6 and decrease of omega-3 sources in today’s diets has to do with changes over the last century in the production of meat, poultry, fish and dairy products. Most chickens and cattle today, for instance, are grain-fed instead of pasture-fed. Since grasses and leafy green plant material is substantially higher in omega-3 fatty acids, beef from pasture-fed cattle will contain two to six times more omega-3 than that from grain-fed beef. Therefore, grain-fed livestock consumption adds to the imbalance between omega-6 and omega-3 fatty acids, but consuming grass-fed livestock improves the balance of the right fats in the diet. Also, the yolks of eggs from cage-free chickens, allowed to eat naturally as God intended, are twice as rich in omega-3 content (and protein) as are commercially produced eggs. Even salmon, a popular and excellent source of omega-3, is often farm-raised, meaning that it is fed from omega-6 sources and is no longer a rich source of omega-3.
beef from pasture-fed cattle will contain two to six times more omega-3 than that from grain-fed beef. Therefore, grain-fed livestock consumption adds to the imbalance between omega-6 and omega-3 fatty acids, but consuming grass-fed livestock improves the balance of the right fats in the diet. Also, the yolks of eggs from cage-free chickens, allowed to eat naturally as God intended, are twice as rich in omega-3 content (and protein) as are commercially produced eggs. Even salmon, a popular and excellent source of omega-3, is often farm-raised, meaning that it is fed from omega-6 sources and is no longer a rich source of omega-3.
The Connection with Obesity and High Insulin Levels
There also is a clear relationship between inflammation and elevated blood sugar levels that stem from diets containing too many refined carbohydrates and sugar. High insulin levels increase the production of arachidonic acid which, in turn, leads to the creation of pro-inflammatory prostaglandins. Unfortunately, it also inhibits the production of prostaglandins that help the body do its work of healing tissues. Another causal factor of both insulin resistance and systemic inflammation is fat tissue packed around abdominal organs, typically referred to as “belly fat.” Recent research has revealed that these types of fat cells, which only increase in size rather than number, generate large amounts of powerful inflammatory substances known as cytokines. Scientists from Washington University School of Medicine in St. Louis discovered some of the first evidence of a link between abdominal fat and systemic inflammation in 2007. Various scientific, medical and nutritional journals cite clear linkage between high levels of these inflammatory markers, raised insulin levels due to blood sugar imbalance and obesity-induced inflammation.
Another causal factor of both insulin resistance and systemic inflammation is fat tissue packed around abdominal organs, typically referred to as “belly fat.” Recent research has revealed that these types of fat cells, which only increase in size rather than number, generate large amounts of powerful inflammatory substances known as cytokines. Scientists from Washington University School of Medicine in St. Louis discovered some of the first evidence of a link between abdominal fat and systemic inflammation in 2007. Various scientific, medical and nutritional journals cite clear linkage between high levels of these inflammatory markers, raised insulin levels due to blood sugar imbalance and obesity-induced inflammation.
Diet plays a significant role in the association between inflammation and obesity in several ways. Not only do all the refined carbohydrates and sugar promote weight gain, but calories from saturated fats and omega-6 sources also convert to fat more readily than do calories from anti-inflammatory omega-3 and omega 9 sources.
Anti-inflammatory Diet Recommendations
It is not just the unhealthy sugars, refined grains and fats that are responsible for shifting most people’s diets to a pro-inflammatory state over the last several generations. Enormous amounts of processed foods, loaded with sugars, trans fats, refined grains, salt, additives, and preservatives have had a major bearing on today’s nutrient deficiencies. Industry experts estimate that 90% of most household food budgets go towards the purchase of these highly processed foods that contain very little but empty calories. It is no wonder that many people’s bodies are deficient in the vitamins and minerals needed for a healthy immune response as well as in antioxidants to neutralize damaging free radicals. An inflammatory state will easily continue and increase without enough fresh, natural whole foods, grown in mineral rich soil, available to supply the right balance of plant nutrients needed for the body to properly heal.
It is no wonder that many people’s bodies are deficient in the vitamins and minerals needed for a healthy immune response as well as in antioxidants to neutralize damaging free radicals. An inflammatory state will easily continue and increase without enough fresh, natural whole foods, grown in mineral rich soil, available to supply the right balance of plant nutrients needed for the body to properly heal.
An anti-inflammatory diet should include an abundance of fresh fruits and vegetables (preferably organic), lean protein sources (free-range poultry, organic eggs, grass-fed beef, wild game and cold-water fish), nuts, seeds, spices and herbs (particularly ones with anti-inflammatory properties like turmeric and ginger) and healthy oils and fats (extra virgin olive oil, organic butter, etc.). It is very important to avoid sugar and high fructose corn syrup, refined grains, grain-fed meats and fish and conventional cooking oils as well as shortening, margarine or anything with hydrogenated or partially hydrogenated fats. Dairy products should be limited and avoided if they create an allergic response. Gluten, found in wheat and several other grains, is a common allergic trigger that can produce inflammation and may also need to be avoided.
It is especially important to identify and avoid food allergens, as many people are unaware that a food allergy may be triggering inflammation and causing their symptoms. I would highly recommend that you read Jack Challam’s book “The Inflammation Syndrome – the Complete Nutritional Program to Prevent and Reverse Heart Disease – Arthritis – Diabetes – Allergies – Asthma” for more specific information on how to discover and avoid triggers related to diet that produce chronic inflammation and disease in the body. His book covers in great detail an “anti-inflammation syndrome” diet plan in addition to an “anti-inflammation syndrome” supplement plan. He also gives many other insights and much good information on how to cool the fires of inflammation in the body and avoid many disease conditions in the process.
His book covers in great detail an “anti-inflammation syndrome” diet plan in addition to an “anti-inflammation syndrome” supplement plan. He also gives many other insights and much good information on how to cool the fires of inflammation in the body and avoid many disease conditions in the process.
Conclusion
Instead of the ongoing use of drugs that block key enzymes and interfere with tissue healing and rebuilding, it is far wiser to support the body’s innate healing ability by resetting the natural immune balance and providing the right conditions for that balance to thrive. When the proper balance of nutrients and dietary fats are restored through eating the right type of foods and taking the correct supplements, the body can indeed regain its natural ability to control inflammation. Look again at the list of triggers to inflammation and begin today to make choices that will reduce or even eliminate from your life the fuels that flame the fire of disease-producing inflammation in your body so that you might enjoy a healthier future.
Sources:
The Inflammation Syndrome by Jack Challem
Stopping Inflammation – Relieving the Cause of Degenerative Diseases by Dr. Nancy Appleton
Inflammation – The Match that Lights All Disease by Steven Horne and Dr. Kimberly Balas
The Ultra Mind Solution by Dr. Mark Hyman
http://www.vaildaily.com/article/20090706/AE/907039954
http://www.womentowomen.com/inflammation/whatischronicinflammation.aspx
http://www.womentowomen.com/inflammation/naturalantiinflammatories.aspx
http://ezinearticles.com/?Inflammation---Could-Inflammation-Be-the-Underlying-Cause-of-Many-Major-Diseases?&id=1558648
http://www.americanheart.org/presenter.jhtml?identifier=4648
http://common-patient-ailments.suite101.com/article.cfm/how_inflammation_occurs
http://www.healthcentral.com/diabetes/c/17/73865/inflammation-root
http://www.bartonpublishing.com/blog/body-weight-inflammation-fat-cell-leakage/?action=print
http://newsblaze.com/story/20051101224906nnnn.nb/topstory.html
http://www.jci.org/articles/view/29069/version/1
Copyright © 2008-2015 Lucinda Bedogne, CNHP, CNC
Post Your Comment...
|
|
||||||||||||


